The year 2025 marks a turning point in medicine, not because of a single discovery, but because of how healthcare systems worldwide have completely re-engineered their methods.
Traditional, paperwork-heavy, and reactive care has given way to predictive, data-driven, and highly personalized systems.
Diagnostics no longer wait for symptoms; treatments adjust themselves automatically; and the line between home and hospital has blurred. Innovation hasn’t just replaced old methods; it has rewritten what modern medicine means.
From AI-powered diagnosis to genetic-level therapies, the healthcare model of 2025 is built on precision, prevention, and patient autonomy.
AI and Machine Learning Replace Manual Diagnostics
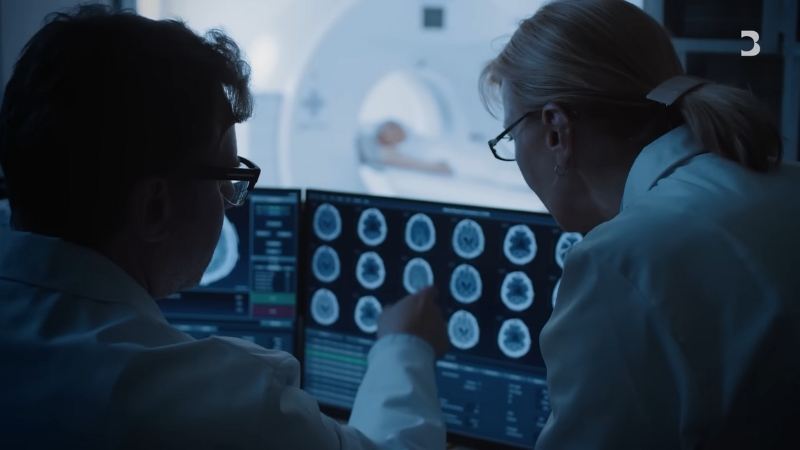
For decades, diagnosis relied on the expertise of doctors interpreting scans, lab results, and patient histories. In 2025, artificial intelligence does this faster and with remarkable accuracy.
Machine learning models now read X-rays, MRIs, and CT scans in seconds, flagging abnormalities even skilled specialists might overlook. Instead of replacing doctors, AI acts as a tireless second set of eyes.
Hospitals across the United States, the UK, and Japan have integrated AI radiology assistants that cut diagnostic time by 70%. In oncology, AI-driven image recognition can now detect early-stage tumors as small as 2 millimeters, often before symptoms appear.
These systems use real-time learning from global datasets, continuously improving accuracy through exposure to millions of cases.
The result: fewer misdiagnoses, faster treatment decisions, and more consistent quality of care. Where once specialists spent hours analyzing scans, they now use that time to focus on patient communication and care planning.
Technology
Previous Method
Innovation Replacing It
Result
Radiology interpretation
Manual visual inspection
AI-driven imaging algorithms
Faster, more precise diagnoses
Lab analysis
Human-processed samples
Automated pathology with machine learning
Reduced human error, 24/7 operation
Patient triage
Paper-based or nurse-led
Predictive AI symptom checkers
Shorter ER wait times, better prioritization
Wearable Health Devices Replace Periodic Checkups
Annual checkups used to be the standard; today, constant monitoring has replaced them. Smartwatches, biosensors, and connected wearables now deliver continuous streams of data to cloud platforms, alerting patients and physicians to early warning signs.
For example, glucose-monitoring patches for diabetics now sync with AI nutrition apps that automatically adjust meal plans. Cardiac patients use smart bands that detect irregular rhythms before they become emergencies.
And sleep-tracking headbands analyze oxygen levels and brain waves, helping detect early sleep apnea without lab visits.
Instead of reactive treatment, healthcare has become proactive. Data analysis identifies risk trends, prompting action before illness progresses. Insurance companies even offer lower premiums to clients who share wearable data, effectively rewarding prevention.
Device
Key Function
Old Method Replaced
Core Benefit
Smart ECG watches
Continuous heart monitoring
Annual ECG at clinics
Early detection of cardiac irregularities
Glucose patches
Real-time blood sugar data
Finger-prick testing
Noninvasive and automatic
AI sleep trackers
Nightly oxygen and REM monitoring
Hospital-based sleep studies
Comfortable, long-term analysis
3D Printing and Personalized Medicine

Mass-produced medical devices and one-size-fits-all treatments are fading fast. In their place, 3D printing and pharmacogenomics are ushering in hyper-personalization. Prosthetics, dental implants, and even bone scaffolds are now custom-printed using patient-specific scans.
This shift cuts production costs and surgery time while improving comfort and recovery outcomes.
In pharmaceuticals, labs are using genetic data to create bespoke medications — compounds optimized for an individual’s DNA and metabolism. These treatments reduce side effects and boost efficacy, moving healthcare away from broad-spectrum medication toward precision therapy.
One of the most striking developments is in bioprinting, where living cells are layered to create tissue for testing or even transplantation. Researchers in Sweden and South Korea are now using 3D-printed liver tissue to study drug toxicity, dramatically improving preclinical safety stages.
Area
Old Method
Innovative Replacement
Outcome
Prosthetics
Mass-produced limbs
3D-printed anatomical models
Faster recovery, better fit
Drug testing
Generic compounds
DNA-matched formulations
Personalized efficacy
Transplants
Donor scarcity
Bioprinted tissue and organs
Reduced waiting lists
Virtual Care Replaces In-Person Follow-Ups
Telemedicine, which began as a pandemic necessity, has evolved into a permanent structure in 2025. Modern healthcare networks use virtual platforms for post-operative checkups, chronic condition monitoring, and even mental health therapy. Patients upload vitals, talk to doctors via video, and receive instant digital prescriptions.
What’s different now is integration. Virtual care platforms link directly with hospital EHRs (Electronic Health Records), wearables, and diagnostic AI systems.
A patient recovering from heart surgery can have daily virtual rounds while their data automatically updates to the hospital cloud.
This hybrid model saves time, reduces hospital congestion, and improves access in rural or underserved regions. For doctors, it means more accurate follow-ups based on real-time data instead of self-reported symptoms.
The Transformation of Clinical Trials
Even clinical trials, once one of the most time-consuming and geographically limited stages of medical research, have been transformed. In 2025, decentralized trials powered by AI recruitment tools and digital consent forms will enable participation from anywhere in the world.
Wearable sensors transmit real-time patient data, while blockchain ensures secure data sharing and traceability.
This new model replaces the old paper-heavy process with adaptive systems that monitor results in real time, allowing faster drug approvals. Companies can now run trials with thousands of participants across continents without requiring centralized testing sites.
The result is faster discovery, greater diversity in participants, and more transparent data integrity, all while cutting costs by up to 40%.
Genomics and Regenerative Therapies Replace Symptom Management
Old healthcare models often focused on treating symptoms, pain, inflammation, or infection, rather than curing underlying causes. Genomic analysis and regenerative medicine are changing that.
By mapping individual genomes, clinicians can identify predispositions to diseases like Alzheimer’s or cancer long before symptoms appear.
Regenerative therapies go further, using stem cells and CRISPR-based gene editing to repair or replace damaged tissue. Clinical applications in 2025 include spinal cord repair, cartilage regeneration, and partial restoration of pancreatic function in diabetic patients.
What was once science fiction is now standard medical research.
Field
Previous Approach
Innovative Technique
Long-Term Benefit
Gene therapy
Post-diagnosis treatment
Preventive genome editing
Eliminates hereditary disease risk
Organ failure
Transplant dependency
Stem-cell regeneration
Self-healing tissue
Cancer therapy
Chemotherapy
Immunogenetic precision therapy
Fewer side effects, targeted action
Conclusion
Modern healthcare in 2025 is defined by replacement, not of people, but of outdated systems. Innovation has moved medicine from reactive to predictive, from generalized to personalized, and from human limitation to data-powered precision.
AI handles diagnostics, wearables manage prevention, genomics personalizes treatment, and digital platforms connect patients and doctors in real time.
The healthcare system of today doesn’t just treat illness; it anticipates it. By merging clinical intelligence with human compassion, innovation has not only replaced old methods but fundamentally reshaped what “healthcare” means in the 21st century.
Related Posts:
- The Latest Machine Learning Trends Shaping Real…
- Who Is the 19-Year-Old Billionaire? Clemente Del…
- The Price Tag on Healthcare - What’s Really Driving…
- Top 15 Modern Architectural Wonders in the World
- Professions Likely to Be Replaced by AI by the End of 2035
- 8 Latest Advances in Hair Transplant Technology for 2024